Major drug insurers like United Health Group, CVS Health, and Humana make estimate bids to Medicare for reimbursement for the cost of Part D prescription drug benefits. From 2006 until 2015 the Wall Street Journal examined industry records and found that insurers reaped an additional $9 billion from overestimates of drug insurance costs.
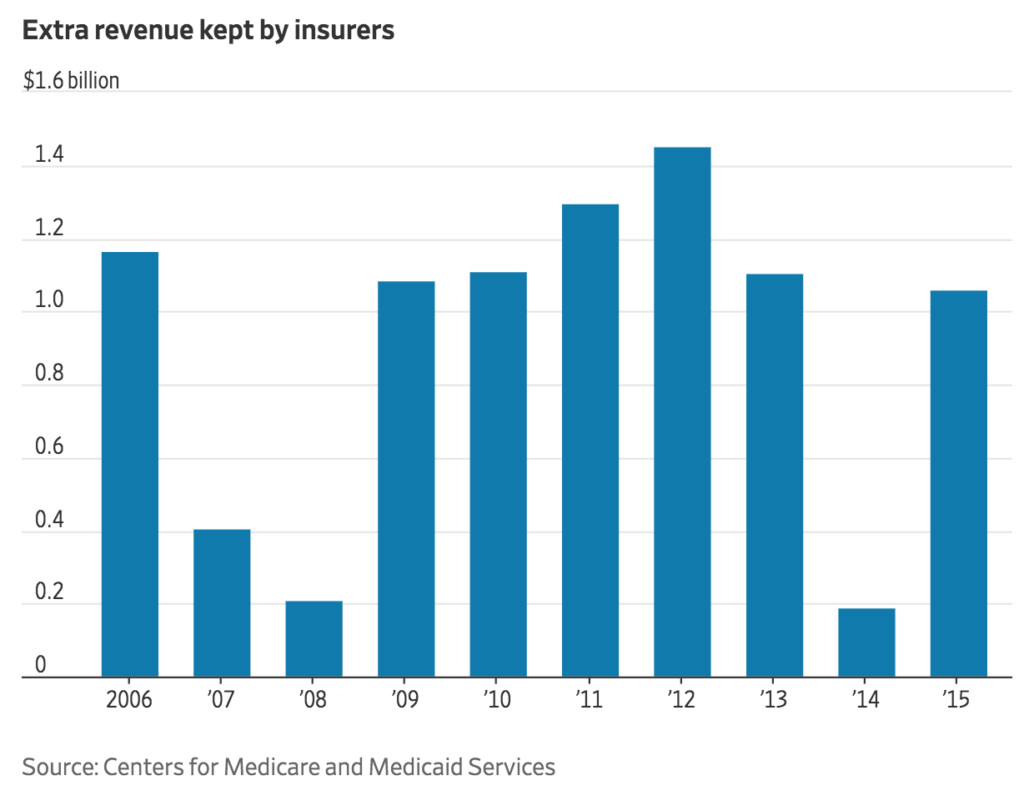
From 2010 to 2017 overall Part D spending rose faster than all other Medicare components by 49 %. The bids from insurers include their profit margins and administrative costs. Medicare reimburses the firms monthly. When the year ends, Medicare audits the estimate totals versus the actuals and requests the overpayments be returned. However, the way the payment terms are setup the insurers are not required by pay the full amount of the overestimate. In 2015 insurers overestimated their Part D costs by $2.2 billion and were allowed to keep $1.06 billion.
The size and continuous overestimate pattern seems unusual. The overestimates are extraordinary to the tune of a million to one according to Memorial Sloan Kettering analysts who completed record examinations for The Wall Street Journal. Peter Bach, director of Sloan Kettering’s Center for Health Policy and Outcomes, noted, “Insurance companies use heaps of data to predict future spending. If truly unpredictable events were blowing up their statistical models, the proportion of overestimates to underestimates would be closer to 50/50.” Dr. Bach concluded, “If they start missing in one particular direction over and over they are doing it on purpose.”
The chronic overestimates are particularly a problem in the direct subsidy part of the program as the following chart shows versus the reinsurance program where estimates are far more accurate.
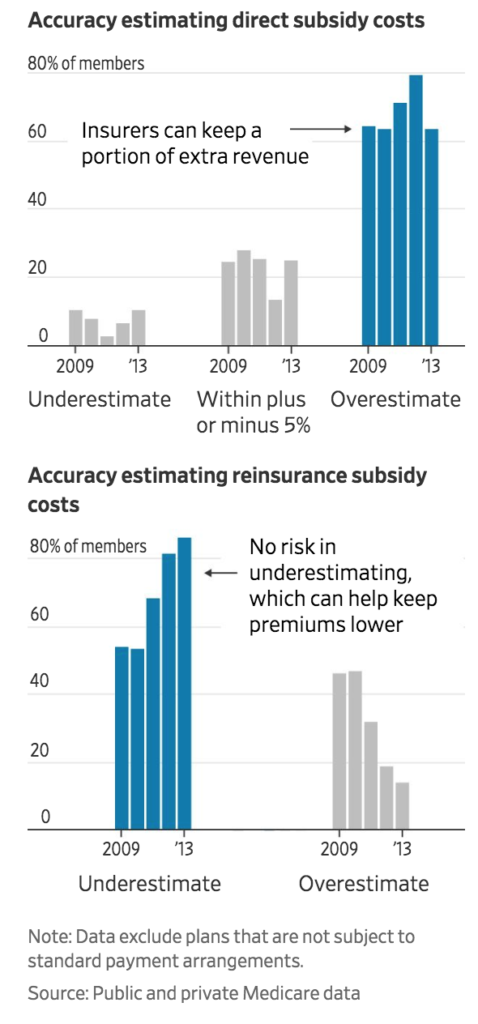
Congress designed the program in 2003 where the federal government and seniors would pay for drug insurance while the program would be operated by private companies. Legislators were concerned that insurers would not want to participate so they allowed for companies to hold back overestimated reimbursement funds. The private companies bear all the risk in the direct subsidy program, yet in the reinsurance program for high cost drugs Medicare bears the risk on underestimates causing losses.
Insurers can gain major benefits by overestimating on the routine drug costs they cover. Companies can keep any overestimated funds up to 5 % of their guess. In some cases they can keep more than 5 % based on a Medicare formula. Medicare steps in if the insurers experience a greater than 5 % loss in their estimate.
Next Steps:
From 2006 to 2015 Medicare spent $652 billion on the Part D program, with its cost increasing by 49 % over that period. Costs must be controlled by private insurers to keep premiums low for seniors and cost overruns limited for the federal government. There is too much reward built into the present direct subsidy program. Why not do as many corporations do for contracts that estimate costs and then must be reconciled at the end of the year? Return all the funds that are overestimated. Chronic overestimating companies would be hit with a penalty for overestimating reimbursement based on the opportunity cost of funds over reimbursed monthly payments. Medicare should reward the accurate estimating companies with positive ratings on their prices, and make clear who the violators are. Making the programs more competitive would bring down costs and require that companies be more accurate in their drug reimbursement estimates.
We see the pricing of drugs via insurers and pharmacy benefit companies as being too opaque to clearly design a fair pricing system. Congress needs to pass a ‘simple pricing’ sunshine bill to make drug pricing clear and accurate for all consumers and the government. Medicare should be able to use its leverage covering millions of seniors to negotiate a reduction in drug and insurance costs. California announced today a policy just signed by the newly installed governor, Gavin Newson, authorizing the California Medicaid administration to negotiate drug prices for all 13 million patients enrolled as a block and invites private employers to join the block. Drug companies and insurers need to shift their focus to make pricing programs more equitable for patients and payers or the face increased calls for price regulation.
